Dr. Amritha Kanakamedala presented an interesting case from here at the VA of an elderly male with a history of spinal stenosis s/p recent surgery 1 week prior to presentation who presented with 1 day of sudden and progressively worsening bilateral hand swelling, pain, erythema, and discoloration.
This case ended up being quite the diagnostic dilemma. The patient had noted violaceous lesions on the palmar surface of his hands initially with associated erythema, swelling, pain and pruritis, but these lesions ended up becoming more dusky colored over time with significantly worsening swelling. He denied any recent medication changes, lotions, clothes, or other exposures. No pets, recent outdoor excursions, or known tick/insect bites. Other than the symptoms mentioned, he denied any systemic symptoms or other symptoms at all. He had never experienced symptoms like this previously.
The patient then developed a fever to 103 F and a similar but new rash on his back on hospital day
A representative image is below:
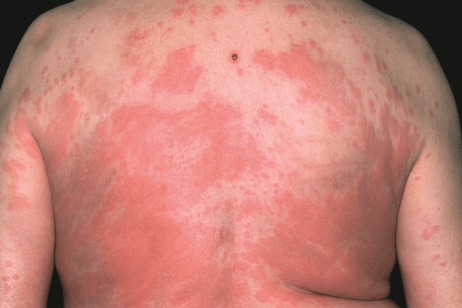
Image obtained from The Pharmaceutical Journal
Dermatology was consulted, and a punch biopsy of the skin of the left palm revealed perivascular lymphocytic infiltrate with abundant eosinophils and neutrophils, consistent with a dermal hypersensitivity reaction. Ultimately, this was felt to possibly due to a delayed drug-related hypersensitivity reaction to perioperative cefazolin that the patient had received. The patient also had a broad infectious and autoimmune workup pending that was ultimately unrevealing. The patient received a short oral corticosteroid course and had near complete resolution of his rash and other symptoms within 2 days and was discharged.
The teaching points of this case are centered around cephalosporin hypersensitivity reactions, which can be distinguished by immediate and delayed reactions.
- Immediate reactions – typically IgE-mediated and onset usually within one hour of dose
- Once sensitization occurs, symptoms may occur at the end of a longer treatment course or with the first dose of a subsequent treatment course
- Include urticarial reactions, angioedema, and anaphylaxis
- If occurs, should avoid all cephalosporins and penicillins until evaluated by an allergist
- Delayed reactions – more common, typically begin after six hours to days after receiving a medication, and generally not IgE-mediated
- Mainly include mild maculopapular skin eruptions, drug fever, and delayed-onset urticaria +/- angioedema
- More severe delayed reactions: Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis (SJS/TEN), Drug reaction with eosinophilia and systemic symptoms (DRESS), and serum sickness like reactions (presents with fever, rash, and arthralgias), and others
- Management of a non-severe delayed reaction, which does not include urticaria or angioedema (requires an allergist evaluation), typically includes avoidance of the drug in the future. With a history of this type of reaction, a cephalosporin can be administered again if it is a superior treatment for a condition in a challenge procedure, coordinated by an allergist. However, more often, a cephalosporin with a different side chain structure is used when presented with these situations.
- Major take home point: A detailed history is key – as illustrated by this case – and thorough review and documentation of medications and allergies is always warranted! Also, any drug reaction should always be updated in the patient’s chart!
References:
- Kelkar PS, Li JT. Cephalosporin allergy. N Engl J Med 2001; 345:804.
- Demoly P, Adkinson NF, Brockow K, et al. International Consensus on drug allergy. Allergy 2014; 69:420.
- Romano A, Gaeta F, Valluzzi RL, et al. Diagnosing nonimmediate reactions to cephalosporins. J Allergy Clin Immunol 2012; 129:1166.
- Lin YF, Yang CH, Sindy H, et al. Severe cutaneous adverse reactions related to systemic antibiotics. Clin Infect Dis 2014; 58:1377.
- Cramp E, Hamilton R, Kerr F, Powell N. Accurately diagnosing antibiotic allergies. The Pharmaceutical Journal, July 2018, Vol 301, No 7915, online | DOI: 10.1211/PJ.2018.20205068